Day 1 :
Keynote Forum
Eckhard U Alt
Technical University of Munich, Germany Tulane University, USA
Keynote: Can we revert the loss of cardiomyocytes in heart failure?
Time : 09:10-09:50

Biography:
Abstract:
Despite revascularization and improved drug therapy, some patients with post myocardial infarction experience a critical loss of functional myocardium leading to remodeling and progression towards heart failure. As the heart is a terminally differentiated organ, renewal and replacement of dead myocardial cells occurs through the intrinsic regenerative potential situated in every organ. As recent research has revealed, the regenerative power of pluripotent stem cells is located throughout the body in small vessels, these cells are able to differentiate into all of the three germ layers. In addition, in every organ we find so-called progenitor cells, which in the heart also constitute the reserve army to replace dying myocardial cells. In light of heart failure with increased ischemia and the survival rate of myocardial cells is significantly reduced, representing an increased turnover and challenge to the stem cells located within the heart. As the ability for stem cells to divide is limited to about 50 to 70 divisions by the telomeres, the regenerative potential in a heart can be exhausted and the functional consequence is a replacement of parenchyma (cardiomyocyte) by fibrous tissue (mesenchyme). Up to now the global understanding why and how cardio myocytes can be replaced is controversial and by most physicians, scientists, and patients obscured. However, the principal of universal stem cells within the body allows obtaining stem cells from one organ, which is not critical such as adipose tissue, to isolate those stem cells and to apply them to the organ in need. The local microenvironment guides the new stem cells through a differentiation program and enables cells to obtain the properties of new cardiomyocytes that completely integrate and synchronize with existing myocardium. The mechanisms of differentiation follow exactly the embryonic differentiation pass way. Hence, it is possible to renew cardiomyocytes by autologous, early stem cells such as the ones that can be retrieved from the stroma of adipose tissue. The mechanism and epigenetic steps of differentiation including results on myocardial regeneration will be presented.
Image:
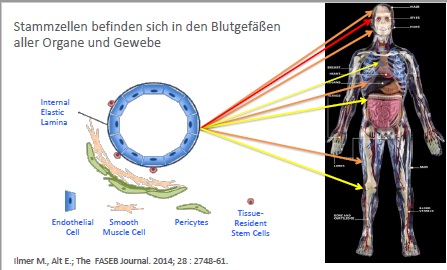
Stem cells reside in virtually all post-natal organs and tissues.
References :
1. Valina, C., Pinkernell, K., Song, Y. H., Bai, X., Sadat, S., Campeau, R. & Alt, E. (2007). Intracoronary administration of autologous adipose tissue-derived stem cells improves left ventricular function, perfusion, and remodelling after acute myocardial infarction. European heart journal, 28(21), 2667-2677.
2. Sadat, S., Gehmert, S., Song, Y. H., Yen, Y., Bai, X., Gaiser, S., ... & Alt, E. (2007). The cardioprotective effect of mesenchymal stem cells is mediated by IGF-I and VEGF. Biochemical and biophysical research communications, 363(3), 674-679.
3. Bai, X., Yan, Y., Song, Y. H., Seidensticker, M., Rabinovich, B., Metzele, R., ... & Alt, E. (2009). Both cultured and freshly isolated adipose tissue-derived stem cells enhance cardiac function after acute myocardial infarction. European heart journal, ehp568.
4. Song, Y. H., Gehmert, S., Sadat, S., Pinkernell, K., Bai, X., Matthias, N., & Alt, E. (2007). VEGF is critical for spontaneous differentiation of stem cells into cardiomyocytes. Biochemical and biophysical research communications, 354(4), 999-1003.
5. Alt, E., Yan, Y., Gehmert, S., Song, Y. H., Altman, A., Gehmert, S., ... & Bai, X. (2011). Fibroblasts share mesenchymal phenotypes with stem cells, but lack their differentiation and colonyâ€forming potential. Biology of the Cell, 103(4), 197-208.
6. Bai, X., & Alt, E. (2010). Myocardial regeneration potential of adipose tissue-derived stem cells. Biochemical and biophysical research communications, 401(3), 321-326.
7. Bai, X., Ma, J., Pan, Z., Song, Y. H., Freyberg, S., Yan, Y., ... & Alt, E. (2007). Electrophysiological properties of human adipose tissue-derived stem cells. American Journal of Physiology-Cell Physiology, 293(5), C1539-C1550.
8. Bai, X., Yan, Y., Coleman, M., Wu, G., Rabinovich, B., Seidensticker, M., & Alt, E. (2011). Tracking long-term survival of intramyocardially delivered human adipose tissue-derived stem cells using bioluminescence imaging. Molecular Imaging and Biology, 13(4), 633-645.
9. Ilmer, M., Vykoukal, J., Boiles, A. R., Coleman, M., & Alt, E. (2014). Two sides of the same coin: stem cells in cancer and regenerative medicine. The FASEB Journal, 28(7), 2748-2761.
10. Alt, E., Pinkernell, K., Scharlau, M., Coleman, M., Fotuhi, P., Nabzdyk, C., ... & Song, Y. H. (2010). Effect of freshly isolated autologous tissue resident stromal cells on cardiac function and perfusion following acute myocardial infarction. International journal of cardiology, 144(1), 26-35.
11. Alt, E. U., Senst, C., Murthy, S. N., Slakey, D. P., Dupin, C. L., Chaffin, A. E., ... & Izadpanah, R. (2012). Aging alters tissue resident mesenchymal stem cell properties. Stem cell research, 8(2), 215-225.
Keynote Forum
Aris Lacis
University Children Hospital, Latvia
Keynote: Possible therapeutic use of stem cells in wide spectrum of pathologies
Time : 09:50-10:30

Biography:
Aris Lacis is a Cardiac Surgeon and Professor. He completed his MD, PhD and Graduation at Riga Medical Institute. He was a General and Thoracic Surgeon at P. Stradina University Hospital in Riga (1964-1969); Thoracic and Cardiac Surgeon at Latvian Centre for Cardiovascular Surgery (1969-1994). From 1994-2012, he was the Head of Pediatric Cardiology and Cardiac Surgery Clinic at University Children’s Hospital, Riga and; since 2012, he has been a Consulting Professor of this Clinic. He is a Vice President of Latvian Society for Cardiovascular Surgery and; President of Latvian Association for Pediatric Cardiologists. He is an Author of 395 scientific publications, three monographs and 13 patents. He is an Investigator in more than 10 clinical trials including cardio surgical procedures performed under deep hypothermia and hybrid procedures etc.
Abstract:
Context: The promising field of regenerative medicine is working to restore structure and function of damaged tissues and organs. The adult heart represents an attractive candidate for cell-based technologies. While there is a wealth of preclinical and clinical data showing the safety, feasibility, and efficacy of stem cells in adults with acute myocardial infarction and heart failure, less is known about possible implementation of stem cell therapy in infants and children with heart failure due to dilated cardiomyopathy and pulmonary arterial hypertension. The challenges facing cardiac stem cell therapy are multiple. There are uncertainties around the destiny of stem cells after their injection into the blood stream. In particular, it regards migration and homing of implanted cells in the target tissues. As yet unclear is the possible role of sympathetic nervous system in the context of osteoreflexotherapy. There is still no definitive answer to the question on which is the preferred type of stem cells to be used for transplantation in different settings. Since 2008, when we first used autologous bone marrow-derived mononuclear cells (BM-MNCs) in patient with acute myocardial infarction, we have investigated the use of stem cells not only for myocardial regeneration in adults and pediatric patients, but also in adult patients with diabetes mellitus and osteoarthritis.
Aim: Aim of this study is to determine the role of BM-MNCs in management of wide spectrum of pathologies, including critically ill pediatric patients, adult patients with acute myocardial infarction & heart failure and adult patients with osteoarthritis.
Design, Settings & Participants: Two patients (9 and 15 years old) with trisomy 21 and severe pulmonary arterial hypertension due to uncorrected large ventricular septal defects received intrapulmonary BM-MNCs implantation. Radionuclide scintigraphy showed improvement of lungs vascularization during 36 months follow-up. Seven patients (four months–17 years) with dilated idiopathic cardiomyopathy received intra myocardial BM-MNCs injections. During follow-up (up to seven year), we observed improvement of left ventricular ejection fraction (LVEF), decrease of left ventricular end diastolic dimension by echocardiography and cardio-thoracic index at chest X-ray exams, reduction of serum brain-natriuretic peptide serum levels and decrease of the stage of heart failure from stage IV to stage I, by NYHA classification. No peri-procedural harmful side effects were observed. We performed BM-MNCs intracoronary infusion in 101 adult patients with acute myocardial infarction with reduced LVEF and in 14 patients with chronic heart failure. Our results showed statistically significant improvement in LVEF at 12 months. We also infused BM-MNCs to the pancreas directly via branches of splenic artery or superior pancreaticoduodenal artery; we have performed single intra-articular BM-MNCs injections in 70 patients with knee or hip joint osteoarthritis (stage II–III). No adverse effects after the BM-MNC injection were observed. Preliminary analysis showed decrease in pain and other symptoms and statistically significant improvement by clinical scoring system using different questionnaires.
Conclusions: The results are promising and we suggest that BM-MNCs might be used for the stabilization of the adult and pediatric patients to improve symptoms and outcomes or serve as a bridge for heart or lung transplantation or delay joint replacement surgery. It also could be recommended in cases if other more traditional treatment options fail or contraindicated.
Keynote Forum
Wei Hua
Fuwai Hospital & Cardiovascular Institute, China
Keynote: The clinical outcome of cardiac resynchronization therapy in dilated-phase hypertrophic cardiomyopathy
Time : 10:50-11:30

Biography:
Wei Hua is a Professor of Cardiology, Deputy Director at Cardiac Arrhythmia Center, Fuwai Hospital & Cardiovascular Institute, Chinese Academy of Medical Sciences, Peking Union Medical College, China. He completed his MD at Shanghai Medical University in 1985 and then PhD at Graduate School of Peking Union Medical College. He joined Fuwai Hospital & Cardiovascular Institute in 1985 and became full Professor of Cardiology in 1999. He was trained in Cardiac Pacing and Electrophysiology in Royal Melbourne Hospital, Australia, from 1994-1996. His main work is on “Clinical cardiac pacing and electrophysiology, cardiac arrhythmias service”. He is now Vice Chairman of Chinese Society of Pacing and Electrophysiology (CSPE) and Chairman of Cardiac Pacing Committee of CSPE. He is a Fellow of Heart Rhythm Society (FHRS), European Heart Rhythm Association (EHRA) and New York Academy of Sciences.
Abstract:
Statement of the Problem: Clinical trials have demonstrated that cardiac resynchronization therapy (CRT) is effective in patients with non-ischemic cardiomyopathy. However, patients with dilated-phase hypertrophic cardiomyopathy (DHCM) have been generally excluded from such trials. We aimed to compare the clinical outcome of CRT in patients with DHCM, idiopathic dilated cardiomyopathy (IDCM) or ischemic cardiomyopathy (ICM).
Methodology & Theoretical Orientation: A total of 312 consecutive patients (DHCM=16; IDCM=231; ICM=65) undergoing CRT in Fuwai hospital were studied respectively. Response to CRT was defined as reduction in left ventricular end-systolic volume (LVESV) ≥15% at six-month follow-up.
Findings: Compared with DHCM, IDCM was associated with a lower total mortality [hazards ratio, HR: 0.35 (95% confidence interval, CI 0.13-0.90)], cardiac mortality [HR: 0.29 (95% CI 0.11-0.77)] and total mortality or heart failure (HF) hospitalizations [HR: 0.34 (95% CI 0.17-0.69)], independent of known confounders. Compared with DHCM, the total mortality, cardiac mortality and total mortality or HF hospitalizations favored ICM but were not statistically significant. [HR: 0.59 (95% CI 0.22-1.61); HR: 0.59 (95% CI 0.21-1.63); HR: 0.54 (95% CI 0.26–1.15) respectively]. Response rate to CRT was lower in the DHCM group than the other two groups although the differences didn't reach statistical significance.
Conclusion & Significance: Compared with IDCM, DHCM was associated with a worse outcome after CRT; the clinical outcome of DHCM patients receiving CRT was similar to or even worse than that of ICM patients. These indicate that DHCM behaves very differently after CRT.
Image:
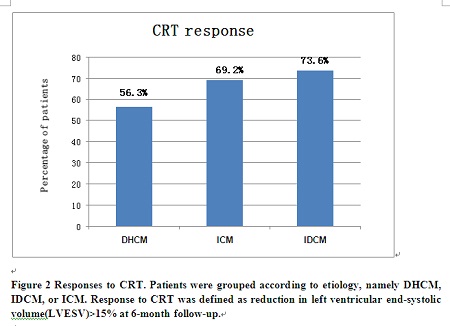
REFERENCES:
1. Hua W, Zhang LF, Wu YF, et al.( 2009) Incidence of sudden cardiac death in China: analysis of 4 regional populations. J Am Coll Cardiol. Sep 15;54(12):1110-8.
2. Yi-Zhou Xu, Yong-Mei Cha, Dali Feng, Wei HUA, et al.( 2012) Impact of Myocardial Scarring on Outcomes of Cardiac Resynchronization Therapy: Extent or Location? J Nucl Med 2012; 53:47-54
3. Hua wei. (2010)Cardiac resynchronization therapy for chronic heart failure in China:guideline and practice(Editorial).Chinese Medical Journal ,123(17): 2293-2294.
4. HUA Wei, HONGXIA Niu, XIAOHAN Fan, et al. (2012) Preventive Effectiveness of Implantable Cardioverter Defibrillator in Reducing Sudden Cardiac Death in the Chinese Population: A Multicenter Trial of ICD Therapy versus Non-ICD Therapy. JCE, 2012, 23(S1): S5-S9
5. HUA Wei, WANG Dong-mei, CAI Lin, et al. (2012) A prospective study to evaluate the efficacy of an intracardiac electrogram-based atrioventricular and interventricular intervals optimization method in cardiac resynchronization therapy. Chinese Medical Journal. 2012, 125(3): 428-433
- Heart Diseases and Heart Failure | Cardiovascular Medicine| Cardiac Surgery and Angiography| Cardiac Arrythmias and Clinical Electrophysiology | Case Study on Cardiology
Location: London, UK

Chair
Lingfang Zeng
Kings College London, UK

Co-Chair
Sherif A S A Mansour
Ain Shams University, Egypt
Session Introduction
Sunny Po
University of Oklahoma Health Sciences Center, USA
Title: Autonomic neuromodulaiton to treat atrial fibrillation
Time : 11:30-12:00

Biography:
Sunny Po is a Cardiac Electro-physiologist and has his expertise in “The effects of the autonomic nervous system on cardiac arrhythmias”. He has discovered that simultaneous activation of the sympathetic and parasympathetic nervous system plays a great role in triggering atrial fibrillation. He also pioneered the therapy of using low-level vagal stimulation at the strength not slowing the sinus rate or atrioventricular conduction to treat atrial fibrillation.
Abstract:
Atrial fibrillation (AF) is the most commonly encountered arrhythmia. Catheter or surgical ablation, aiming at isolating the pulmonary veins to eliminate the triggers and substrate of AF is the therapy of choice for drug-refractory AF. Despite the advances of the ablation technologies, the success rate of AF ablation remains disappointing. It is evident that pulmonary vein isolation (PVI) is not enough to treat even the earliest stage of AF, paroxysmal AF, not to speak more advanced stages of AF. It is known that simultaneous activation of the sympathetic and parasympathetic nervous system plays a major role in the initiation and maintenance of AF. Interventions targeting these neural elements have been shown to favorably affect the clinical course of AF. Multiple preclinical studies demonstrated that low-level vagal stimulation at the strength not slowing the sinus or atrio-ventricular conduction was capable of suppressing AF initiation as well as terminating AF. Injection of botulinum toxin into major atrial ganglionated plexi, the integration centers of the cardiac autonomic nervous system, not only prevented post-operative AF in paroxysmal AF patients undergoing open-heart surgeries but also significantly suppressed the progression of AF in these patients. Recently, a novel therapy by transcutaneous stimulation of the auricular branch of the vagus nerve demonstrated its efficacy on shortening the AF duration, prolonging the atrial effective refractory period as well as suppressing the inflammatory markers such as TNF-α and CRP in paroxysmal AF patients undergoing AF ablation. Results of these recent clinical studies indicate that autonomic neural modulation may be a novel and noninvasive therapy for patients suffering from drug-refractory AF.
References :
1. Qin M, Liu X, Jiang WF, Wu SH, Zhang XD, Po SS. Vagal response during pulmonary vein isolation: Re-recognized its characteristics and implications in lone paroxysmal atrial fibrillation. Int J Cardiol. 2016 May 15;211:7-13.
2. Lo LW, Chang HY, Scherlag BJ, Lin YJ, Chou YH, Lin WL, Chen SA, Po SS. Temporary Suppression of Cardiac Ganglionated Plexi Leads to Long-Term Suppression of Atrial Fibrillation: Evidence of Early Autonomic Intervention to Break the Vicious Cycle of "AF Begets AF". J Am Heart Assoc. 2016 Jul 5;5(7).
3. Zhang L, Po SS, Wang H, Scherlag BJ, Li H, Sun J, Lu Y, Ma Y, Hou Y.Autonomic Remodeling: How Atrial Fibrillation Begets Atrial Fibrillation in the First 24 Hours. J Cardiovasc Pharmacol. 2015 Sep;66(3):307-15.
4. Yu L, Dyer JW, Scherlag BJ, Stavrakis S, Sha Y, Sheng X, Garabelli P, Jacobson J, Po SS. The use of low-level electromagnetic fields to suppress atrial fibrillation. Heart Rhythm. 2015 Apr;12(4):809-17.
5. Gao M, Zhang L, Scherlag BJ, Huang B, Stavrakis S, Hou YM, Hou Y,Po SS. Low-level vagosympathetic trunk stimulation inhibits atrial fibrillation in a rabbit model of obstructive sleep apnea. Heart Rhythm. 2015 Apr;12(4):818-24.
6. Stavrakis S, Humphrey MB, Scherlag BJ, Hu Y, Jackman WM, Nakagawa H, Lockwood D, Lazzara R, Po SS. Low-level transcutaneous electrical vagus nerve stimulation suppresses atrial fibrillation. J Am Coll Cardiol. 2015 Mar 10;65(9):867-75.
7. Huang B, Yu L, Scherlag BJ, Wang S, He B, Yang K, Liao K, Lu Z, He W, Zhang L, Po SS, Jiang H. Left renal nerves stimulation facilitates ischemia-induced ventricular arrhythmia by increasing nerve activity of left stellate ganglion. J Cardiovasc Electrophysiol. 2014 Nov;25(11):1249-56.
8. Pokushalov E, Kozlov B, Romanov A, Strelnikov A, Bayramova S, Sergeevichev D, Bogachev-Prokophiev A, Zheleznev S, Shipulin V, Salakhutdinov N, Lomivorotov VV, Karaskov A, Po SS, Steinberg JS. Botulinum toxin injection in epicardial fat pads can prevent recurrences of atrial fibrillation after cardiac surgery: results of a randomized pilot study. J Am Coll Cardiol. 2014;12;64(6):628-9.
9. Katritsis DG, Pokushalov E, Romanov A, Giazitzoglou E, Siontis GC, Po SS, Camm AJ, Ioannidis JP. Autonomic Denervation Added to Pulmonary Vein Isolation for Paroxysmal Atrial Fibrillation: A Randomized Clinical Trial. J Am Coll Cardiol. 2013, 62(24):2318-25.
Paul H Wooley
Kardiatonos Inc., USA
Title: A novel model of atherosclerosis in mice
Time : 12:00-12:30

Biography:
Paul H Wooley is the Chief Scientific Officer at Kardiatonos Inc., USA. He completed his PhD in Immuno-genetics at Guys Hospital Medical School. He was a Mayo Clinic Fellow and a Professor at Wayne State University, Wichita State University and KU Medical School, USA.
Abstract:
Porphyromonas gingivalis have been found in atherosclerotic lesions in humans. We developed a murine model of atherosclerosis using a 60% fat diet and gavage of PCB-77 and/or atherosclerotic lesions in humans. We developed a murine model of atherosclerosis using a 60% fat diet and gavage of PCB-77 and/or P. gingivalis. The model was assessed by histological examination of the aortic sinus, and ELISA assays for biomarkers of damage to the endothelial glycocalyx. C57/BL6 mice were raised from six weeks on either regular diet or a 60% fat diet. PCB-77 and/or P. gingivalis (ATCC 33277) suspensions were administered by oral gavage and mice sacrificed on days 10, 15 or 20. Frozen sections were cut through the aortic valve and analyzed for the presence and size of plaques, amount of fibrous tissue and inflammation. ELISA test kits measured thrombin-anti-thrombin complex, anti-thrombin III, total plasminogen activation inhibitor-1, syndecan 1, heparan sulfate and hyaluronan synthase 1. Animals receiving one PCB-77 gavage and one bacterial gavage demonstrated a low level of fibrous tissue and fat staining with a moderate level of inflammation. Fat staining was observed in foam cells in the artery walls of two sections in the aortic sinus with cholesterol inclusions. Most mice receiving three gavages of PCB-77 showed a moderate level of fat staining with low inflammation. Significantly higher levels of PAI-1 in mice were receiving one PCB-77 gavage and one bacterial gavage than in the control group. Levels of heparan sulfate detected in mice receiving three gavages of PCB-77 were significantly higher than in the control group. The levels of syndecan 1 and hyaluronan synthase 1 in the mice receiving three gavages of PCB-77 were significantly higher than in controls. The data show that administration of PCB and P. gingivalis to mice fed a high fat diet resulted in pathological features and biomarker abnormalities indicative of the presence of cardiovascular disease.
Image:
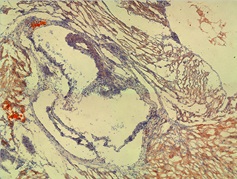
Figure shows an area of foam cells in the wall of the sinus containing lipid staining in mice receiving two gavages of PCB-77 and one gavage of bacteria.
References.
1. Fukasawa, A., Kurita-Ochiai, T., Hashizume, T., Kobayashi, R., Akimoto, Y., & Yamamoto, M. (2012). Porphyromonas gingivalis accelerates atherosclerosis in C57BL/6 mice fed a high-fat diet. Immunopharmacology and immunotoxicology,34(3), 470-476.
2. Arsenescu, V., Arsenescu, R. I., King, V., Swanson, H., & Cassis, L. A. (2008). Polychlorinated biphenyl-77 induces adipocyte differentiation and proinflammatory adipokines and promotes obesity and atherosclerosis.Environmental health perspectives, 116(6), 761.
Lingfang Zeng
King's College London, UK
Title: A histone deacetylase 7-derived 7-amino acid peptide acts as a phosphorylation carrier
Time : 12:30-13:00

Biography:
Lingfang Zeng has his expertise in Stem Cell Research in Vascular Biology field, specifically on Mechanotransduction, Epigenetic Modification and Alternative Splicing. He has done extensive investigation on HDAC3, HDAC7 and IRE1α/XBP1 signal pathway. His current research focuses on Alternative Translation. His group found that small open reading frame within so-called non-coding area or non-coding RNA could be translated to produce functional small peptides. In addition to ATG, they found that other codons could also initiate the translation to produce more small peptides.
Abstract:
Histone deacetylase 7 (HDAC7) belongs to the class II HDAC family and plays a pivotal role in the maintenance of endothelium integrity. There are eight splicing variants in mouse HDAC7 mRNAs. Within the 5’ terminal non-coding area of some variants, there exist some short open reading frames (sORFs). Whether these sORFs can be translated or resulting peptides play roles in cellular physiology remain unclear. In this study, we demonstrated that one sORF encoding a 7-amino-acid (7-aa) peptide could be translated in vascular progenitor cells (VPCs). Importantly, this 7-aa peptide (7A) could transfer the phosphate group from the phosphorylated Ser393 site of MEKK1 to the Thr145 site of 14-3-3γ protein. The phosphorylated 7A (7Ap) could then directly phosphorylate 14-3-3γ protein in a cell-free, in-gel buffer system. The adjacent histidine and proline residues are essential for the phosphate group reception and transfer. In vitro functional analyses revealed that 7A and 7Ap increased VPC self-renewal and migration and enhanced vascular endothelial growth factor (VEGF)-induced VPC migration and differentiation toward the endothelial cell (EC) lineage, in which MEKK1 and 14-3-3γ served as the upstream kinase and downstream effector, respectively. Knockdown of either MEKK1 or 14-3-3γ attenuated VEGF-induced VPC migration and differentiation. Exogenous 7Ap could rescue the effect of VEGF on the MEKK1 siRNA-transfected VPCs but not on the 14-3-3γ siRNA-transfected VPCs. In vivo studies revealed that 7A, especially 7Ap, induced capillary vessel formation in matrigel plug assays, increased re-endothelialization and suppressed neointima formation in the femoral artery injury model, and promoted foot blood perfusion recovery in the hind limb ischemia model by increasing Sca1+ cell niche formation. These results indicate that the sORFs within the non-coding area can be translated and that 7A may play an important role in cellular processes such as proliferation, migration and differentiation by acting as a phosphorylation carrier.
References:
1. Yang J, et al (2016) Analysis of histone deacetylase 7 alternative splicing and its role in embryonic stem cell differentiation toward smooth muscle lineage. Methods Mol Biol. 1436:95-108.
2. Zhou B, et al (2011). Splicing of histone deacetylase 7 modulates smooth muscle cell proliferation and neointima formation through nuclear β-catenin translocation. Arterioscler Thromb Vasc Biol. 31(11):2676-84
3. Zhang Let al (2010). Sp1-dependent activation of HDAC7 is required for platelet-derived growth factor-BB-induced smooth muscle cell differentiation from stem cells. J Biol Chem. 285:38463-72
4. Margariti A, et al (2010). Histone deacetylase 7 controls endothelial cell growth through modulation of beta-catenin. Circ Res. 106:1202-11.
5. Margariti A, et al (2009). Splicing of HDAC7 modulates the SRF-myocardin complex during stem-cell differentiation towards smooth muscle cells. J Cell Sci. 122:460-70.
Mridula Dhakad
Saudi German Hospital, Dubai
Title: Newer treatments in heart failure
Time : 14:00-14:30

Biography:
Mridula Dhakad is a senior interventional Cardiologist with more than 25 years of experience in Interventional and Clinical Cardiology. She has actively participated in many national and international conferences. She has been extensively involved in treating many complex and critical cardiac patients. She has received her interventional training at well reputed large public and private hospitals. She did her fellowship in Interventional Cardiology at a world renowned large volume centre at Paris. She was instrumental in establishing Cardiology department at various reputed institutions. She is an active member of European Society of Cardiology and a life member of Cardiology.
Abstract:
Fight against reducing the disability in heart failure patients is on and tremendous advancements in management of such patients with low ejection fraction over past few decades has improved the prognosis. Wealth of research data is available on this, wherein the scientists have delved deep into studying the apoptosis of myocytes and how the failing cells can be brought back into function by targeting the maladaptive neurohormonal pathways. Across the spectrum of the heart failure patients, the following range of pharmacotherapy prescribed over the past years has definitely lowered the hospital admission rates and prolonged survival but still the readmission rates are high and financial burden on the healthcare systems are alarming–diuretics, renin-angiotensin-aldosterone system inhibitors, B-blockers, digoxin and vasodilators being the mainstay of therapy. The discovery of two new classes of drugs has marked a new beginning in the care of chronic heart failure patients. Ivabradine and sacubitril/valsartan seem to be promising agents in improving the functional capacity and quality of life, reducing the hospital readmission rates and mortality. They reduce the stress on the myocardium by reducing the heart rate and improve the blood flow by relaxing the vessels thereby improving clinical outcomes. End stage heart failure patients still queue up for heart transplantation worldwide but lack of available donors necessitates them to use ventricular assist devices (like LVAD) as a bridge therapy in capable centers. ECMO also has been used for short term circulatory support. The key focus in this talk will be on novel drug treatment for systolic heart failure.
Jianrui Song
University of Michigan, USA
Title: Myeloid-specific IL4 receptor alpha knockout increases adverse cardiac remodeling post myocardial infarction
Time : 14:30-15:00

Biography:
Jianrui Song is a PhD candidate in Cell and Developmental Biology at University of Michigan. She has received her Master’s Degree from China in 2009, where she worked on “The role of autophagy in hypoxic microenvironment and chemo- and radiotherapy in liver cancer”. As a PhD candidate, she is pursuing training in the field of Cardiovascular Disease and Immunology. She is working on how myeloid cells participate in the response of cardiac ischemia, the formation of infarct and the post infarct response, and also in determining how altering myeloid (especially macrophage) phenotype by IL4Ra can affect these responses in order to identify processes that can be targeted for beneficial effect. She is supported by the Bradley Merrill Patten Research Fellowship and by an American Heart Association Pre-doctoral Fellowship.
Abstract:
Myocardial infarction (MI) elicits inflammatory reactions that are orchestrated by a wide range of immune cells including macrophages. Reprogramming macrophages towards a resolving and reparative phenotype is a potential therapeutic approach for MI. However, how to modify macrophages in order to improve cardiac injury is not clear. Interleukin 4 receptor alpha (IL4Ra) activation is one of the major alternative activated macrophage (also names M2 macrophage) inducers, so IL4Ra is a potential macrophage modifier. Here, we knocked out IL4Ra from myeloid cells to determine how IL4Ra signaling is involved in cardiac remodeling post MI. Myeloid-specific IL4Ra knockout (MyIL4RaKO) did not show significant change in cardiac hypertrophy and interstitial fibrosis. There was decreased infarct size at one week post MI, but by three weeks there was no significant difference in infarct size. We saw significantly increased infarct thickness and perivascular fibrosis at three weeks, indicating the involvement of IL4Ra signaling in cardiac remodeling. Importantly, along with these significant changes in cardiac remodeling, MyIL4RaKO mice showed significantly decreased cardiac function at three weeks post MI. IL4Ra signaling was significantly inactivated in macrophages; however no change was shown in macrophage polarization in heart tissues post MI. In conclusion, IL4Ra signaling in myeloid cells is critical in maintaining proper cardiac remodeling and cardiac function post MI, which suggests the potential of modifying macrophages through enhancing IL4Ra signaling as a therapeutic strategy for MI.
References :
1.Manabu Shiraishi, Yasunori Shintani, Yusuke Shintani, Hidekazu Ishida, Rie Saba, et al, and Ken Suzuki. Alternatively activated macrophages determine repair of the infarcted adult murine heart. J Clin Invest. 2016 Jun 1;126(6):2151-66.
2.Janine Woytschak, Nadia Keller, Carsten Krieg, Daniela Impellizzieri, Robert W. Thompson, et al, and Onur Boyman. Type 2 Interleukin-4 Receptor Signaling in Neutrophils Antagonizes Their Expansion and Migration during Infection and Inflammation. Immunity. 2016 Jul 19;45(1):172-84.
3. Johanna A. Knipper, Sebastian Willenborg, Ju¨ rgen Brinckmann, Wilhelm Bloch, Tobias Maaß, et al, and Sabine A. Eming.Interleukin-4 Receptor alpha Signaling in Myeloid Cells Controls Collagen Fibril Assembly in Skin Repair. Immunity. 2015 Oct 20;43(4):803-16.
4.Slava Epelman, Kory J. Lavine, Anna E. Beaudin, Dorothy K. Sojka, Javier A. Carrero, Boris Calderon, Thaddeus Brija, Emmanuel L. Gautier, Stoyan Ivanov, Ansuman T. Satpathy, Joel D. Schilling, et al, and Douglas L. Mann. Embryonic and adult-derived resident cardiac macrophages are maintained through distinct mechanisms at steady state and during inflammation. Immunity. 2014 Jan 16;40(1):91-104.
5.Michael G. Usher, Sheng Zhong Duan, Christine Y. Ivaschenko, Ryan A. Frieler, Stefan Berger, Günther Schütz, Carey N. Lumeng, and Richard M. Mortensen. Myeloid mineralocorticoid receptor controls macrophage polarization and cardiovascular hypertrophy and remodeling in mice. J Clin Invest. 2010 Sep;120(9):3350-64.
Niraj Khatri Sapkota
Chitwan Medical College- Tribhuvan University, Nepal
Title: Waist circumference is strong predictor of hypertension in male
Time : 15:00-15:30

Biography:
Niraj Khatri Sapkota has completed his PhD in Molecular Physiology applications to pharmacology at the age of 32 years from Zhejiang University, China, one of the Thomson Reuters and Elsevier best ranked university of the world; he is now working as an Associate Professor in the Department of Physiology in Chitwan Medical College affiliated to Tribhuvan University, Nepal. He is an active researcher and academician of his country, Nepal. He has published more than 50papers both original and review papers as a single author or with collaboration in reputed international journals and is serving as a reviewer, advisory and editorial board member and Editor of more than 30 international reputed journals.
Abstract:
Hypertension is one of the cardiovascular variables raised state, systolic and diastolic blood pressure are its parameters that can be easily measured, alteration of blood pressure is commonly observed in different condition, but persistent elevated state is one of the alarming remark of the cardiovascular biology, therefore status of blood pressure in the adult in different anthropometric measures are adopted but especial focus is given to waist circumference at different anatomical site said to be one of the indicator of adiposity depots that is associated with cardio metabolic risk.
Aims: Hence, this study aims to find whether addition of waist circumference (WC) to body mass index (BMI; kg/m2) play additive or strong independent role in predicting health risk than does BMI alone.
Methods: A community based cross sectional study was conducted by incorporating total of substantial number (more than 100) of subjects in the data who were male only older than 25 years, non smokers, non alcoholic, didn’t have history of taking any type of medication, non vegetarian with normal physical activity and were residents in the urban and rural areas throughout, were included in the present study. Waist circumference referenced to umbilicus measured by non tensile and non flexible measuring tape and at the mean time height and weight were also recorded by standard device in order to calculate BMI and blood pressure was measured by Aneroid sphygmomanometer of the respective subject subsequently data analysis was made by using SPSS to compare the BMI and Waist circumference relationship with blood Pressure independently to identify their relationship with hypertension.
Results: Keeping few exceptional aside, Both BMI and Waist Circumference exhibited positive association with blood pressure, while the waist circumference was more strongly associated with hiking of blood pressure and also BMI is not always the relating parametric tool to metabolic disease as was conventionally considered.
Conclusion
The result and analytical data showed that (P<0.05) there is significant strong correlation of blood pressure with waist circumference comparatively more than BMI thus WC alone can significantly predict the co-morbidity therefore this study approach to suggest and hints to follow as a routine task for measuring Waist circumference while taking inference for diagnosing hypertension risk at least in male.
Reem Kayyali & Aliki Peletidi
Kingston University London, UK
Title: Contribution of pharmacists in cardiovascular disease prevention journey
Time : 15:30-16:00

Biography:
Reem Kayyali completed her Pharmacy Degree at Nottingham University; MSc in Bio-pharmacy at King’s College London and; PhD in the Management of Thalassaemia. She was awarded the Maplethorpe fellowship for two years at King’s College London. After that, she worked for four years as a Research Fellow at University College London Medical School. In 2006, she joined Kingston University and now is an Associate Professor and the Director of Research and Enterprise in the School of Life Sciences, Pharmacy and Chemistry. Her current research interests are focused on “Medicines optimization, public health and technology enabled care”.
Aliki Peletidi completed her Pharmacy Degree at Kingston University London. Currently, she is pursuing her PhD about the role of pharmacists in cardiovascular disease prevention.
Abstract:
Statement of the Problem: Cardiovascular disease (CVD) is the primary cause of death worldwide causing 29.6% in 2010. In the UK, CVD was the second cause of mortality, responsible for 27% deaths in 2014 and 48% of all deaths in Greece in 2012. CVD is a result of risk factors such as hypertension, dyslipidemia, overweight/obesity, stress, smoking, physical inactivity and diabetes. CVD prevention consists of two stages: Primary and secondary. Pharmacists, one of the most accessible healthcare professionals, do not have a clear role in the existing pathways. In our view, there are three prevention stages: Primary, secondary and tertiary. The primary prevention constitutes enhancing awareness and initial screening of the public for CVD risk factors (obesity, lack of exercise, alcohol misuse and tobacco use) in order to estimate their CVD risk. Pharmacists could offer services such as weight management, alcohol brief intervention, smoking cessation and health checks. Secondary prevention is the management of post-diagnosis risk conditions (diabetes, hypertension and dyslipidemia) in order to prevent the incidence of a CVD disease. At this stage, pharmacists could provide services with a view to optimize medicines to improve medication adherence and to offer lifestyle advice. Tertiary prevention is the linkage between prevention and treatment for those who already suffered a CVD episode with a view to decreasing the risk of a secondary episode or mortality.
Methodology & Theoretical Orientation: A qualitative study utilizing semi-structured interviews with UK and Greek pharmacists was undertaken to explore their current and future roles in CVD prevention. The conceptual framework used was based on the results of the literature search conducted on the pharmacist's role in CVD risk factors and conditions. The interview schedule, which included 28 questions in three sections, was designed based on the proposed CVD prevention pathway. Purposive sampling was used, obtaining 40 participants in total for both countries.
Results: The analysis identified the following themes; role recognition and priority services. Both UK and Greek pharmacists played a role in secondary prevention, after risk conditions have been diagnosed. They are eager to monitor patients’ blood pressure or blood glucose when necessary, and provide lifestyle advice when they dispense the prescribed medications to them. Furthermore, in Greece it was identified that pharmacists had an appetite to initiate CVD prevention services. Pharmacists were willing to start a weight management programme to help their clients to reduce their CVD risk. Therefore, a weight management service was designed and is currently being evaluated.
Conclusion & Significance: This study identified UK and Greek pharmacists’ perspectives on their role in CVD prevention. Pharmacists’ role is mainly focused in secondary and less in primary and tertiary CVD prevention. However, in Greece, pharmacists recognized a potential role in primary prevention and early screening of CVD. There is a need of more work targeted in tertiary prevention to reduce complications and the chance of a secondary or a third CVD episode as well as premature mortality.
References :
1. Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, Abraham J, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380:2095–2128.
2. Townsend N, Bhatnagar P, Wilkins E, Wickramasinghe K, Rayner M. Cardiovascular disease statistics 2015, British Heart Foundation: London.
3. World Health Organization. Greece: Noncommunicable Diseases (NCD) Country Profiles. Available from: http://www.who.int/nmh/countries/grc_en.pdf [Accessed: 16th October 2016].
4. Peletidi A, Nabhani-Gebara S, Kayyali R. Smoking Cessation Support Services at Community Pharmacies in the UK: A Systematic Review. Hellenic Journal of Cardiology 2016; 57: 7-15.
5. Yusuf S, Hawken S, Ounpuu T, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case control study. The Lancet. 2004; 364: 937–52.
6.Hobbs F. Cardiovascular Disease: Different Strategies for Primary and Secondary Prevention?. Heart 2004; 90:1217–1223.
Andrey V Kuznetsov
Innsbruck Medical University, Austria
Title: Cytoskeleton and regulation of mitochondrial function: The role of beta-tubulin II and plectin
Time : 16:15-16:45

Biography:
Andrey V Kuznetsov has worked on the problems of delicate mechanisms of energy metabolism in the heart and their changes under pathophysiological conditions. He has studied mitochondrial function and regulation in normal cells and in various pathological states, in particular in the field of mitochondrial cardiac system, mitochondrial interactions with other intracellular structures and systems, performing analysis of mitochondria in situ and in vivo. Also, he studied the roles of mitochondrial damage in ischemia reperfusion injury, apoptosis, calcium homeostasis, oxidative stress, mitochondrial ROS production, cardiac and muscle diseases with imaging of mitochondria and mitochondrial function, mitochondrial dynamics (fission, fusion, motility) in various living cells. He has extensive knowledge in cardiac bioenergetics and mitochondrial physiology and experience in optical imaging (fluorescent, two-photon) of single cell and single mitochondria, imaging of mitochondrial Ca2+, ROS, membrane potential, mitochondrial dynamics for basic science and in clinically oriented studies.
Abstract:
The control of mitochondrial function is a cardinal issue in the field of cardiac bioenergetics, and the analysis of mitochondrial regulations is central to basic research and in the diagnosis of many diseases. Interaction between cytoskeletal proteins and mitochondria can actively participate in mitochondrial regulation. Potential candidates for the key roles in this regulation are the cytoskeletal proteins plectin and tubulin. Analysis of cardiac cells has revealed regular arrangement of β-tubulin II, fully co-localized with mitochondria. β-tubulin IV demonstrated a characteristic staining of branched network, β-tubulin III was matched with Z-lines and β-tubulin I was diffusely spotted and fragmentary polymerized. In contrast, HL-1 cells were characterized by the complete absence of β-tubulin II. Comparative analysis of cardiomyocytes and HL-1 cells with cardiac phenotype revealed a dramatic difference in the mechanisms of mitochondrial regulation. In the heart, colocalization of β-tubulin isotype II with mitochondria suggests that it can participate in the coupling of ATP-ADP translocase (ANT), mitochondrial creatine kinase and VDAC. This mitochondrial supercomplex is responsible for the efficient intracellular energy transfer via the phosphocreatine pathway. We found also that in skeletal muscle of plectin knockout mice, mitochondrial content was reduced; mitochondria were aggregated in sarcoplasmic and subsarcolemmal regions, and were no longer associated with Z-disks. Our results show that the depletion of distinct plectin isoforms (P1b and P1d) affects mitochondrial network organization and function in different ways. Existing data suggest that cytoskeletal proteins may control the VDAC, contributing to the regulation of mitochondrial and cellular physiology.
References:
1. Bagur R, Tanguy S, Foriel S, Grichine A, Sanchez C, Pernet-Gallay K, Kaambre T, Kuznetsov AV, Usson Y, Boucher F, Guzun R. (2016) The impact of cardiac ischemia/reperfusion on the mitochondria-cytoskeleton interactions. Biochim. Biophys. Acta. 1862(6):1159-71.
2. Winter L, Kuznetsov AV, Grimm M, Zeöld A, Fischer I, Wiche G. (2015) Plectin isoform P1b and P1d deficiencies differentially affect mitochondrial morphology and function in skeletal muscle. Human Molecular Genetics. 24(16):4530-44.
3. Kuznetsov AV, Javadov S, Sickinger S, Frotschnig S, Grimm M. (2014) H9c2 and HL-1 cells demonstrate distinct features of energy metabolism, mitochondrial function and sensitivity to hypoxia-reoxygenation. Biochim. Biophys. Acta. 1853(2):276-284.
4. Varikmaa M, Bagur R, Kaambre T, Grichine A, Timohhina N, Tepp K, Shevchuk I, Chekulayev V, Metsis M, Boucher F, Saks V, Kuznetsov AV, Guzun R. (2014) Role of mitochondria-cytoskeleton interactions in respiration regulation and mitochondrial organization in striated muscles. Biochim. Biophys. Acta. 1837(2):232-45.
5. Tepp K, Mado K, Varikmaa M, Klepinin A, Timohhina N, Shevchuk I, Chekulayev V, Kuznetsov AV, Guzun R, Kaambre T. (2014) The role of tubulin in the mitochondrial metabolism and arrangement in muscle cells. J. Bioenerg. Biomembr. 46:421-434.
6. Javadov S, Kuznetsov AV. (2013) Mitochondria: the cell powerhouse and nexus of stress. Frontiers in Physiology. Vol. 4, article 207.
7. Kuznetsov AV, Javadov S, Guzun R, Grimm M, Saks VA. (2013) Cytoskeleton and regulation of mitochondrial function: the role of beta-tubulin II. Frontiers in Physiology. Vol. 4, article 82.
Ahmed N Ghanem
Retired Consultant Urologist, Egypt
Title: Volumetric overload shocks in the pathoetiology of the transurethral resection prostatectomy syndrome and acute dilution hyponatraemia
Time : 16:45-17:15

Biography:
Abstract:
The transurethral prostatectomy syndrome (TURS) is defined as severe vascular hypotension reaction that complicates endoscopic surgery as a result of massive irrigating fluid absorption causing severe acute dilution hyponatremia (HN) of <120 mmol/l. The vascular shock is usually mistaken for one of the recognized shocks and volumetric overload shock type 1 (VOS1) is overlooked making volumetric overload shock type 2 (VOS2) unrecognizable. In adults VOS1 is induced by the infusion of 3.5-5 liters of sodium-free fluids and is known as TURS or HN shock. VOS2 is induced by 12-14 liters of sodium-based fluids and is known as the adult respiratory distress syndrome. The most effective treatment for VOS1 and VOS2 is hypertonic sodium of 5%NaCl or 8.4% sodium bicarbonate. The literature on TURS is reviewed and the underlying pathoetiology is discussed. As Starling’s law for the capillary-interstitial fluid transfer, which underlies the principles of fluid therapy, proved wrong an alternative mechanism was found by studying the hydrodynamics of the porous orifice (G) tube akin to capillary. Incorporating the G tube in a chamber (C), representing the interstitial space surrounding a capillary, demonstrated a rapid dynamic magnetic field-like fluid circulation between the C and G tube lumen. The G-C phenomenon is autonomous having both filtration and absorption forces making a true replacement for Starling’s law in every tissue and organ of the body.
Sherif A S A Mansour
Ain Shams University, Egypt
Title: The value of preoperative administration of aminophylline as a cardio protective agent during coronary artery bypasses grafting
Time : 17:15-17:45

Biography:
Sherif A S A Mansour is a Consultant of Cardiothoracic Surgery in Ministry of Health Hospitals, in addition to working as a Surgeon in Royal Stoke Hospital, Stoke-on-Trent, UK. He works at Ain Shams University in Cairo, Egypt as a Senior Lecturer. He is subspecialized in Off Pump CABG, minimal invasive cardiac surgery with fantastic results and many contributions to various cardiac surgery centers in the Middle East, Asia and Africa. He has publications in the peer reviewed journals and contributions in some published cardiothoracic books with many contributions at international conferences across Europe and Asia. Recently, he started to explore the field of Robotic Heart Surgery with strong steps toward achieving his goal of mastering it.
Abstract:
Objectives: Myocardial ischemic reperfusion injury remains the most uncontrolled aspect of cardiac operations. This study aims at testing the hypothesis that aminophylline could serve as a potential myocardial protector against reperfusion injury during coronary artery bypass grafting (CABG).
Methods: A prospective, randomized, single blinded, placebo - controlled study involving 60 patients divided into two groups. Group A (30 patients) preoperatively received aminophylline, 200 mg orally per day for 3 days with a total dose of 600 mg. Group B (30 patients) was given placebo. All patients underwent uniform pre/intra/post-operative management. Assessment of cardiac markers (Troponin I) and cardiac enzymes were done before induction of anesthesia, after 30 min of aortic cross clamping and postoperatively (1, 24 and 48 hours). Preoperative concentration of aminophylline in serum was measured. Postoperative, 12 lead ECG after 48 hours and echocardiographic full study examination at the 6th day were examined.
Results: Total ICU stay hours and ventilation hours were statistically higher (p-value<0.05) in group B (67.20±21.28 and 16.47±8.76 hours, respectively) than in group A (46.87±14.46 and 12.20±3.56 hours, respectively). The need of inotropes in group A was lower than that in group B in the immediate postoperative period. However, Troponin I and cardiac enzymes in both groups were of no statistical significant difference (p-value>0.05).
Conclusions: Aminophylline may have beneficial role in CABG surgeries by decreasing the ventilation hours, need of inotropic support and total ICU stay hours. However, there was no relevant impact on cardiac marker and enzymes.
Hamid Amer
King Abdulaziz Hospital for National Guards, Saudi Arabia
Title: The significance of ECG changes during adenosine infusion as a stress agent for myocardial perfusion imaging (MPI) in predicting coronary artery disease (CAD)
Time : 17:45-18:15

Biography:
Hamid Amer is Nuclear Cardiology Board Certified and is an Associate Consultant in Nuclear Medicine at King Abdulaziz Hospital for National Guards, Saudi Arabia. He is involved in researches related to the Department of Nuclear Cardiology.
Abstract:
Purpose: The significance of electrocardiographic ECG changes during adenosine stress test is debatable. This study will further elaborate the significance of these changes in predicting the possibility of CAD.
Methods: This was a retrospective observational registry performed in a single center at the Kingdom of Saudi Arabia. The data were collected from the nuclear medicine database identifying all the reported Gated myocardial perfusion SPECT with adenosine stress tests between January 2013 and January 2014. The adenosine dose were fixed with all patients based on body weight and was given as a continuous infusion of 140 mcg/kg/min over a 6-minute period.
Results: There were 346 patients identified with cardiac nuclear scans in the pre-specified time frame who were subjected to adenosine stress scan. 152 of these patients were male accounting for 44% of the total population. Average age at the time of examination was 60.82±11.29 years. Patients were presented with one or more risk factors. Patients with base line abnormalities, past history of CAD with or without PCI or CABG and previous MI were excluded from the study. Ninety-eight patients (28%) were reported as positive for CAD, 40 patients were reported with ischemic ECG changes (12%) during adenosine infusion, 23 patients who have ischemic changes were positive on MPI, while 17 patients who have positive ECG had a negative MPI. Odd Ratio (OR) was 4.16, 95% C.I. was (2.11-8.18). Fisher Exact test was applied and showed a P value of <0.01. No reported case of asystole, myocardial infarction or complete heart block in this study period.
Conclusions: Our study showed that the probability of a positive MPI is 4 times higher with positive ECG ischemic changes during adenosine stress test and consequently these ECG ischemic changes should be taken in consideration in the final report.
